8 clinical implications of elevated C-reactive protein, not just bacterial infections
C-reactive protein (CRP) is an acute-phase response protein induced by interleukin 6 (IL-6) in hepatocytes, with a normal reference value of < 5 mg/L. Advances in testing technology have improved the sensitivity and accuracy of CRP detection. Existing tests can detect very low concentrations of CRP in the serum of a sample, known as hypersensitive C-reactive protein (HS-CRP).CRP is a non-specific marker of inflammation and its elevation does not simply identify bacterial infection. In addition to infection, tissue damage, inflammation and stress can also increase CRP after 6 h, with a peak in 1 to 2 days.
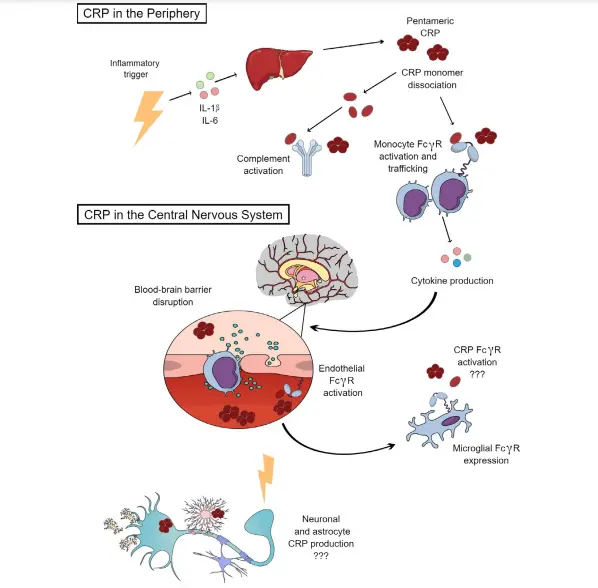
The pathogenesis of CRP in the inflammatory response is complex. As shown in Figure 1, in the peripheral system, inflammatory triggers induce the release of cytokines such as IL-1β or IL-6, and the liver synthesizes CRP. CRP activates the complement system and monocyte FcγR receptors, leading to macrophage activation, transport and induction of the inflammatory signalling cascade. This cascade also triggers activation of endothelial FcγR receptors in the central nervous system (CNS) and upregulation of CRP expression by microglia.
The interaction of CRP with complement C1q and FcTR results in a variety of biological activities, including host defence responses to infection, phagocytosis and regulation of inflammatory responses. Thus, the binding of CRP to damaged cells, apoptotic cells and nuclear antigens allows it to play an important role in autoimmune diseases.
CRP is commonly used as a biomarker of infection or inflammation, and its values are valuable for clinical assessment of the infectious agent, the severity of the patient’s condition, and the identification of infectious or non-infectious disease. When the cause is clear, the rise and fall of CRP is closely related to the appropriateness of therapeutic measures and the determination of disease progression.
CRP is used to determine the pathogen of infection.
In viral infections, CRP is usually normal or mildly elevated, while in bacterial infections, the increase is more pronounced; 80% of bacterial infections have a CRP of >100 mg/L [2].
Other studies have shown that a CRP of <10 mg/L can largely exclude bacterial infection. In those who do have bacterial infections, the mean CRP value for gram-positive infections is 48 mg/L, while CRP values for gram-negative infections are two times higher than those for gram-positive infections [3].
CRP is a reference for assessing the severity of infection and the course of medication.
In definite infections, a serum CRP value in the range of 10-100 mg/L is often indicative of a local or superficial infection; if CRP is ≥100 mg/L, invasive infection or sepsis may be considered [2].A significant decrease in serum CRP compared to the pre-drug level indicates that current anti-infective therapy is effective and the CRP value can be used as a reference to assess the course of anti-infective therapy. Therefore, CRP values can be used to assess the severity of an infected person’s illness, to identify serious infections, and to assess the course of anti-infective therapy for the benefit of the patient.
CRP for the assessment of infectious diseases.
Appendicitis.
The Blok GCGH team [4] retrospectively analysed 1076 cases of children admitted to hospital with acute abdominal pain to investigate the diagnostic value of CRP values in children with appendicitis. The study found that children with CRP < 10 mg/L and abdominal pain for >48 h were less likely to have appendicitis. The sensitivity and specificity of CRP 10 mg/L as the threshold for the initial diagnosis of appendicitis were 0.87 (95% CI, 0.77-0.94) and 0.77 (95% CI, 0.74-0.79) respectively.
Notably, CRP specificity was not high. Non-infectious diseases such as surgery, trauma, autoimmune diseases, tumours and myocardial infarction can also lead to increased serum CRP values.
Non-infectious diseases with elevated CRP.
Pulmonary embolism (PTE).
Serum CRP values in 379 patients with PTE ranged from 0.3 to 813.2 mg/L, with 288 patients having elevated CRP (>10.0 mg/L) and 91 patients having normal CRP (0.1-10.0 mg/L) [5]. Their study suggests that the majority of patients with PTE have elevated CRP values, perhaps in association with CRP promoting blood clotting.
Cardiovascular disease.
CRP is known to promote atherosclerosis, blood clotting and plaque formation, and the pathology of cardiovascular disease includes leukocyte invasion and inflammation of the vascular lining; therefore, patients with cardiovascular disease have higher serum CRP values. It has been suggested that CRP should be included in the catalogue of biochemical indicators for the diagnosis of cardiovascular disease, together with low-density lipoprotein cholesterol (LDL-C) and cholesterol (TC) [6].
Rheumatoid arthritis (RA).
The development of RA is associated with the induction of IL-6, tumour necrosis factor (TNF) and CRP production and release following macrophage and mast cell activation. trends in CRP values in RA patients are relevant for assessing their response to drug therapy, disease progression, etc.
The team of Nawata M[7] recruited 244 RA patients who had been using infliximab for at least 1 year. The subjects’ modified total change score (mTSS) was calculated and the factors were analysed by multivariate logistic regression at the start of treatment (baseline) and 54 weeks after treatment. The trial found that CRP decreased from 1200 mg/L at baseline to 100 mg/L in RA patients treated with infliximab, suggesting that high CRP levels in RA patients during infliximab treatment were an independent predictor of disease progression (e.g. increased joint destruction) and that increases and decreases in CRP values were associated with other autoimmune disease activity and regression of outcome.
Gastric cancer.
Lu J et al. counted 401 patients with gastric cancer before and after radical gastrectomy and performed a multifactorial analysis to explore the independent variable of recurrence-free survival (RFS) in order to assess patient prognosis. This trial showed that preoperative CRP ≥ 3.1 mg/L and postoperative peak CRP values (CRPmax) ≥ 77.1 mg/L were risk factors for RFS in patients with gastric cancer [8].
It is important to note that CRP is elevated in patients with active malignancies. Therefore, routine follow-up of CRP in patients with malignant neoplasms can assist in assessing the progression of their disease.
Acute pancreatitis.
Serum CRP concentrations in patients with severe acute pancreatitis can be ≥ 200 mg/L. The severity of the disease is positively correlated with the CRP value. A CRP value of 210 mg/L was used as a reference value to assess the severity of acute pancreatitis, with a sensitivity of 83% and specificity of 85% [9].
Summary.
This paper has outlined the pathological mechanisms of CRP as a biomarker in infectious or inflammatory reactions, and discussed the clinical value of CRP in determining the pathogen of infection and evaluating the severity of infection. In this paper, we have listed the common diseases that cause an increase in CRP values and hope to provide some suggestions for clinical management.