Bipolar disorder has a higher suicide rate than depression, and early medical attention can reduce the damage
Bipolar disorder is a dysfunctional brain with problems in the transmission of neurosecretory substances. The main cause of the disorder is mostly congenital or originates in the family, and frustrations in life are only triggers.When a person with bipolar disorder has difficulty overcoming stress, he or she may experience symptoms of mania or depression. When the person is depressed, he or she may suddenly feel hopeless and have suicidal thoughts, while when the person is manic, he or she may become exaggeratedly confident, spend money frivolously, have an increased sexual appetite, or even imagine that he or she has divine powers. Patients with bipolar disorder often have a rollercoaster of moods, and their moods fluctuate more easily than those of depressed patients. These mood swings can be very distressing for patients, and they may also abuse drugs and alcohol more than depressed patients, and may also have stronger suicidal tendencies. If you find that someone close to you is experiencing these conditions, you should take the patient to seek medical attention as early as possible. The earlier the patient seeks medical attention, the less damage to the brain can be done, and there have been cases where the patient has already experienced slowed thinking and memory loss when seeking medical attention.
Patient Xiao Ju (female, 20 years old), 4 years history of bipolar disorder.
In 2018, the patient presented with unexplained sleep disturbances, depressed mood, unexplained pessimistic apprehension, did not want to do anything and did not want to go to school, and was diagnosed with depression at that time. After medication, she had hallucinations, heard someone cursing her out of thin air, saw god-like images, suspected that someone was targeting her, talking about her behind her back, felt that someone was trying to harm her, and talked to herself. She was diagnosed with bipolar disorder on a second visit, and was treated with aripiprazole and quetiapine medication. The patient was discharged from hospital and took the medication regularly, but her symptom control fluctuated.
Up to now, the patient has been hospitalized five times, and his psychiatric symptoms can be summarized as follows: manic episodes are characterized by excitement and talkativeness, profligacy, hallucinations, delusions of victimization, feeling of being followed and watched, babbling nonsense with content that others do not understand, abnormal behavior, kowtowing to the wall for no reason, hostility to his parents, hitting his mother and dropping things; depressive episodes are characterized by depressed mood, pessimism and anxiety, self-harm, having taken a large amount of oral medication to commit suicide, and unwillingness to communicate with others. The patient’s family brought him to our department for surgical treatment.
After treatment, the patient’s mood was significantly more stable, he no longer saw strange images or heard non-existent sounds, he had a good attitude when talking to his family and medical staff, his questions and answers were relevant, he was able to recall his past life experiences and family members, he had a clear perception of his current place and time, he admitted that he needed treatment for his illness, and he also promised to take his medication on time and in accordance with his dosage after discharge, and to participate in regular review and rehabilitation.
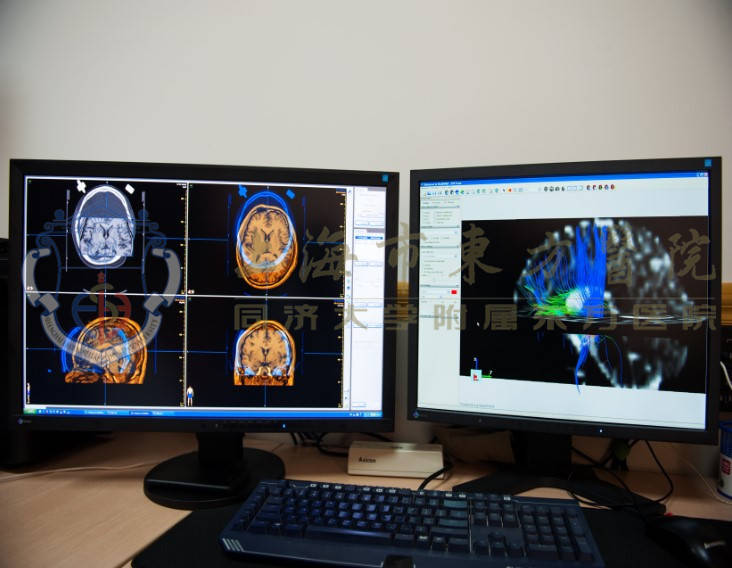
Surgical treatment of refractory bipolar disorder involves the fusion of CT/MRI/DTI and other imaging techniques into a surgical planning and navigation system. The computer will carry out 3D modelling, calculate the location of the target point and simulate the surgical path, and assist the surgeon to make a small incision of about 1-3cm in the patient’s head based on a minimally invasive approach to give targeted neuromodulation to the corresponding nuclei. This directly blocks abnormal nerve signalling, balances abnormal neurotransmitter secretions and restores normal function to the pathological neural circuits, thus helping patients to control or eliminate abnormal psychiatric symptoms.
Therefore, bipolar disorder is not an incurable disease and can be “clinically cured” if the patient continues to receive treatment, medication and, if necessary, surgery, to return to a normal family and social life.



